Camilla Forte/Borderless Magazine/Catchlight Local/Report for America
Camilla Forte/Borderless Magazine/Catchlight Local/Report for AmericaEl Dr. Thaer Ahmad pasó años viajando a Gaza como médico voluntario antes de 2023. Ahora, continúa tratando a pacientes en el South Side de Chicago mientras aboga por los trabajadores de la salud de Palestina.
Esta historia ha contado con el apoyo de la campaña Brave of Us .
El Dr. Thaer Ahmad, palestino-estadounidense, supo que quería ser médico después de ver a su padre lidiar con la enfermedad cardíaca reumática — una complicación de la faringitis estreptocócica que desarrolló cuando tenía 9 años debido a la falta de antibióticos y acceso a atención médica.
“Eso siempre fue algo que me llenó de amargura y resentimiento,” dijo Ahmad. “Que él tuviera que lidiar con eso debido a las circunstancias de la ocupación y el apartheid.”
Esos momentos consolidaron la pasión de Ahmad por la medicina y la ayuda humanitaria a lo largo de los años. Se convirtió en el primero de su familia en poner pie en Gaza en 2009, a los 21 años, y había regresado en cinco ocasiones distintas para el momento en que Israel lanzó sus ataques militares contra palestinos en octubre de 2023.
Noticias que ponen el poder en el punto de mira y a las comunidades en el centro.
Suscríbase a nuestro boletín gratuito y reciba actualizaciones dos veces por semana.
Ahora, radicado en el South Side de Chicago, trabaja como médico de emergencias y ha estado involucrado en labores de ayuda humanitaria por más de una década.
“Sabía que esto iba a ser parte de lo que quería hacer por mucho tiempo,” dijo Ahmad.
Borderless Magazine habló con Ahmad sobre su compromiso con la ayuda humanitaria, sus experiencias como voluntario en Gaza y sus esfuerzos de defensa desde entonces.
Donde todo comenzó
Tenía 4 años cuando mis padres me enviaron a Palestina. Todavía pienso en ese día.
Era 1992, justo hacia el final de la Intifada*. Me quedé con mis abuelos en su casa en un suburbio de Jerusalén y probablemente fue uno de mis primeros recuerdos reales.
Recuerdo el jardín, muy pequeño, enfrente de la casa de mis abuelos. Había una ambiente tenso debido a la Primera Intifada.
Pero fue increíble — conocer a diferentes miembros de la familia allí. Tenemos familia en Chicago, pero la mayoría de nuestra familia vive en el pueblo, allá en Palestina.
Todo el mundo se conoce. Mientras caminas por la calle, alguien te detendrá y te preguntará quién es tu padre o tu madre, y luego te explicará cómo conoce a toda tu familia. Te preguntarán qué parentesco tienen contigo o te hablarán sobre recuerdos de tu infancia que tengan de ti.
Se siente una conexión instantánea.
Se convirtió en una parte muy importante de mi identidad. Realmente comencé a entender lo que significaba cuando usas la frase “allá en casa.”
Mis padres vinieron aquí en los años ochenta desde Palestina, y hemos estado en el área de Chicago desde entonces.
Inicialmente estábamos en el South Side, donde había muchos otros miembros de la diáspora palestina. Luego, lentamente comenzamos a mudarnos más hacia los suburbios del suroeste, donde muchas personas con orígenes similares se estaban reasentando.
A pesar de haber nacido y crecido aquí, ser palestino-estadounidense sigue siendo un proceso muy nuevo que creo muchos de nosotros estamos tratando de descifrar cómo manejar.
La diáspora aquí está asimilando ahora el hecho de que existe la posibilidad de que nunca podamos regresar a nuestro hogar en Palestina. A pesar de eso, la solidaridad y la conexión aún existen entre las personas.
Hubo algunos momentos cruciales que me hicieron querer dedicarme a la medicina. Uno de mis recuerdos centrales fue cuando mi primo de 17 años fue herido de bala y asesinado en Palestina. Era un manifestante desarmado que abogaba por mejores condiciones carcelarias.
Recuerdo estar en el hospital mientras lo operaban. Permaneció en coma hasta que finalmente murió.
Fue una escena que no olvidaré, y todavía recuerdo toda aquel ambiente. Me dejó una impresión duradera.
Con el paso del tiempo, pasé más tiempo en Palestina y me di cuenta de que quería participar en labores de ayuda y desarrollo. Pero me pregunté, “¿Dónde podría ser eficaz y qué papel podría desempeñar para mi gente?”
Sentí que ser médico y estar involucrado en salud global sería de gran impacto.
Tuve la fortuna de participar en una misión de ayuda humanitaria antes de empezar la facultad de medicina. Eso reforzó mi decisión de dedicarme a la medicina y al trabajo humanitario.
Voluntariado en Gaza
La primera vez que fui a Gaza fue en 2009, después de Operación “Plomo Fundido."
Barack Obama ganó la presidencia en noviembre de 2008, y ese mismo día, los israelíes habían llevado a cabo un ataque aéreo, matando a cuatro personas en Gaza. Ese evento condujo posteriormente a la Operación “Plomo Fundido,” en la que entre diciembre de 2008 y enero de 2009, 1.400 palestinos fueron asesinados, incluyendo alrededor de 300 niños.
Recuerdo ese momento muy claramente. Nuestra comunidad quedó devastada por ello. Estábamos protestando en Chicago y en todo EE. UU.
Unos meses después, tuve la oportunidad de unirme a un convoy de ayuda humanitaria que iba de Egipto a Gaza.
Tras muchos retrasos debido al sofocante bloqueo sobre Gaza, pude entrar y vi las zonas que habían sido destruidas y conocí a algunas de las familias. Me paré sobre los escombros donde todavía había cuerpos debajo.
Cuando estalló el genocidio en octubre de 2023, había estado en Gaza cinco veces en diferentes misiones como médico trabajando en hospitales junto a otros trabajadores de la salud palestinos. El enfoque era mejorar el acceso a los recursos, pero también construir un esfuerzo colaborativo entre la diáspora y los trabajadores de la salud locales.
Después del 7 de octubre, se cerraron las fronteras y nadie entraba. Pero en diciembre, nos enteramos de que iban a permitir la entrada de equipos internacionales.
Nos enteramos de que la Organización Mundial de la Salud (OMS, por sus siglas en inglés) estaba buscando voluntarios. Les dije que iba a tener que ser una de esas personas. Y me fui.
A todos los voluntarios se les asignó un hospital — yo iba a estar en el Hospital Nasser en Khan Younis, que está cerca del sur de Gaza. La administración del hospital nos alojó en una habitación del hospital.
Estuve en urgencias, en la sala de reanimación donde envías a los enfermos y heridos en estado crítico. Solía estar con uno o dos médicos palestinos que se estaban formando para ser médicos de urgencias.
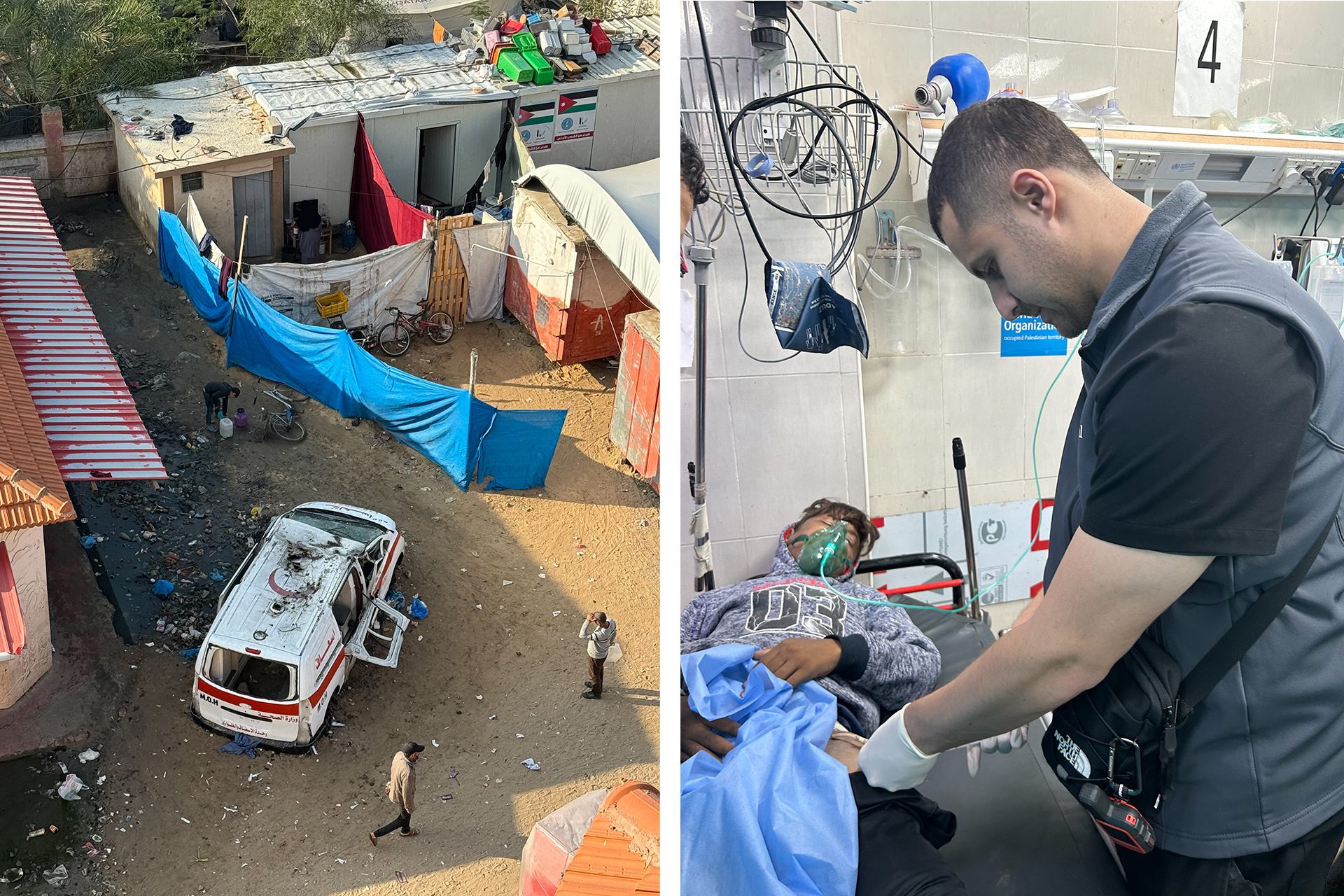
El hospital más grande de Gaza, Al-Shifa, fue rodeado, atacado y ya no funcionaba — quedó fuera de servicio. Nasser se había convertido en el hospital más grande y, por lo tanto, recibíamos pacientes de todas las demás partes de Gaza. Estábamos desbordados, no solo de pacientes, sino también de personas desplazadas.
Cada rincón de este hospital estaba ocupado por alguien que había sido desplazado. Es una escena muy abrumadora para alguien que viene de Estados Unidos. Nunca había visto algo así.
Además, no paraban de llegar pacientes debido a las bombas que se oyen. He estado en Gaza anteriormente cuando los israelíes la bombardearon, pero nunca había oído algo así. Cada vez que escuchas una bomba explotar, sientes la onda expansiva golpear tu cuerpo.
Estaba mirando por la ventana y pude ver cómo cada vecindario y calle era arrasado y destruido. Oleadas de humo se elevaban de los edificios que colapsaban y se acercaba cada día más.
Estoy atendiendo a personas en el suelo y tenemos que realizar procedimientos que nunca he hecho en ese tipo de entorno. Me estaba apoyando mucho en los médicos y enfermeras palestinos de Gaza. Ellos habían estado haciendo esto, en ese momento, durante al menos medio año.
Tuvimos que adaptarnos constantemente según la persona que teníamos delante. Pasábamos de una emergencia caótica a otra emergencia caótica.
Por ejemplo, un día, surge una escasez de fórmula para bebés prematuros para los ocho bebés en la unidad de cuidados intensivos neonatales. Durante los próximos dos días, esa será la emergencia número uno debido a lo peligroso y mortal que es. Luego, una vez que consigamos un poco de fórmula para bebés, de repente, estaremos a una hora de perder todo el combustible diésel del generador que abastece de energía al hospital y a todas las personas conectadas a ventiladores que usan electricidad, niños en incubadoras, personas en cirugía — van a morir.
Con estas limitaciones y el abrumador volumen de pacientes, ¿cómo se determina la asignación de recursos para la atención médica vital?
Una situación en la que me vi involucrado ocurrió cuando bombardearon una casa y trajeron a una familia de 20 personas. Seis de ellas llegaron muertas, pero tres de ellas estaban en sus últimos momentos si no hacíamos algo. Pero solo tuvimos la oportunidad de dedicar estos recursos a una persona.
¿Es ese un escenario imposible en los Estados Unidos? No lo es. ¿Pero sucedería todos los días? No. Eso sucedía todos los días en Gaza.
Esas son el tipo de decisiones desgarradoras que los trabajadores de la salud palestinos estaban tomando todos los días, sin excepción. Puedes imaginar lo que eso hace en términos de daño moral a estos seres humanos que están sirviendo a sus comunidades.
No vienen de los Estados Unidos y poder disfrutar de un respiro después de un mes de trabajo. Se lo están haciendo a diario a personas que se parecen a ellos y hablan como ellos. El simple hecho de que el hospital pudiera funcionar es un testimonio de la capacidad de los trabajadores de la salud palestinos para encontrar maneras de continuar atendiendo a los pacientes.
Encontraron maneras de trabajar. Es algo por lo que no reciben suficiente reconocimiento.

De Gaza a la defensa de derechos
Algunos días, me siento amargado y no sé cómo procesar el hecho de que, si quisiera, podría pedir una resonancia magnética aquí en Chicago y escanear el cuerpo entero de alguien. Eso no ha estado disponible para nadie en Gaza en dos años y medio. Incluso entonces, estaba limitado.
Es algo extraño sentarse detrás de una computadora y poder ordenar cualquier tratamiento o prueba que desees al alcance de tu mano.
Así que creo que parte de mi regreso aquí a los Estados Unidos es asegurarme de que sigo organizando, sigo documentando para el registro histórico lo que ha estado sucediendo, de cualquier manera que pueda.
Una perspectiva positiva es que he podido interactuar con la próxima generación de trabajadores de la salud. No solo en mi institución, sino en todo el país.
Soy subdirector del programa de formación de nuestro hospital para personas que quieren convertirse en médicos de urgencias, así que estoy involucrado en su educación.
Hay una diferencia con esta generación. Están prestando atención y quieren saber qué pueden hacer diferente.
Estos son los futuros líderes de la atención médica en los Estados Unidos y se preocupan por la medicina social aquí. La conectan con la medicina global en el extranjero.
Esa solidaridad va a cambiar nuestra profesión de una manera que tendrá un impacto real a nivel local y global.
Intifada en árabe se refiere a “levantamiento” o “sacudida.” Se refiere a los levantamientos y protestas palestinas contra años de ocupación israelí. La Primera Intifada se marca entre 1987 y 1993.
Tara Mobasher es redactora y reportera del boletín informativo de Borderless Magazine. Envía un correo electrónico a Tara a [email protected]